Featured
-
3.0K7Food Guidelines
Why It Matters if Your Dog Likes Their Food
Anyone with a dog knows they’re hardwired to snack on some pretty icky stuff (cat poop, garbage, dead animals), so when it...
-
3.3K2RALPH Speaks
Top 5 Things to do After the End of the World
I’ve gotta tell you guys, I’m a little excited for the “end of the world.” Of course I’ll miss my human. I...
-
37Funny Dog Posts
Weekly Roundup: Funny Dog Posts From Last Week (Apr 22)
We present you funny dog posts from Apr 14 to Apr 20 that will paws-itively make you through the rest of the...
-
765Canine Rights
Missing Dog Found Wrapped In Duct Tape Gets Rescued And Reunited With Owner
A missing dog found wrapped in duct tape in a dumpster gets rescued by the Nebraska Humane Society (NHS) on Monday, April...
-
64Health & Wellness
Welfare Experts Reveal 10 Dog Features Pet Owners Should Avoid
An international team of experts reveal 10 dog features that future and current dog owners should avoid in a dog to ensure...
-
61Awesome Stories
Introducing BARK Air, A New Airline Designed For Dogs That Will Launch In May
The dog brand BARK announces the launch of a new airline designed to cater to every dog's travel needs — BARK air.
-
59Entertainment
Man Finds Missing Pet Husky Using A Drone, Finds It Hanging Out With A Family Of Bears
A man captures a drone video of his missing Husky hanging out with a family of bears in the forest, and the...
-
58Awesome Stories
A Guide Dog In The UK Nicknamed ‘DogFather’ Retires After Fathering A Total Of 323 Puppies
Guide Dogs UK announces that their guide dog, dubbed as the "Dogfather", is retiring after fathering a total of 39 litters and...
-
57Funny Dog Posts
Weekly Roundup: Funny Dog Posts From Last Week (Apr 15)
We present you funny dog posts from Apr 07 to Apr 13 that will paws-itively make you through the rest of the...
-
983FRONT PAGE
United Airlines Flight To Seattle Is Diverted To Dallas After A Dog Poops In First Class Aisle
A United Airlines flight to Seattle was forced to divert to Dallas after a First Class passenger's dog poops in the aisle...
-
63Lifestyle
Pilot Study Shows Dogs Can Smell Trauma In Human Breath
A recent study found evidence that dogs might be able to "sniff out" the onset of a post-traumatic stress disorder (PTSD) episode...
-
56Dogs With Jobs
Dog Who Failed Police Academy Steals People’s Hearts While Helping Find Quake Victims In Taiwan
A Labrador Retriever in Taiwan failed to become a drug-sniffing dog. Now, he is helping find quake victims after the country suffered...
Dogington Post Reviews
Popular
-
3.0K7Food Guidelines
Why It Matters if Your Dog Likes Their Food
Anyone with a dog knows they’re hardwired to snack on some pretty icky stuff...
-
3.3K2RALPH Speaks
Top 5 Things to do After the End of the World
I’ve gotta tell you guys, I’m a little excited for the “end of the...
-
1.3KAdoption
‘Extremely Special Adoption’: Dog Who Stayed At Shelter For 7 Years Gets Adopted By Woman She Has Touching Ties With
An Animal Resource Center (ARC) shelter dog, who stayed at the shelter for seven...
-
927Skin & Coat
A Beginners Guide To Dog Paw Hyperkeratosis
Does your dog have hairy paw pads? If yes, then it might be suffering...
-
82810Canine Rights
Deputy Who Shot A Missouri Family’s Dog And Threw It In A Ditch Is Being Sued
A deputy from Missouri who shot a family's dog and threw its body in...
-
730Health & Wellness
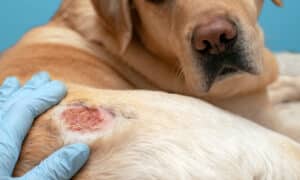
6 Of The Most Common Dog Skin Conditions
Dog skin conditions are very common. As a matter of fact, they are among...
-
6751Health & Wellness
Heat Stroke in Dogs: Breeds Most At Risk This Summer
Summer for dogs is not as fun. As a matter of fact, during this...
-
672Awesome Stories
Lost Dog Survives Epic 150-Mile Journey Across Alaskan Sea Ice And Returns Home
A lost Australian Shepherd, named Nanuq, survives an incredible 150-mile journey across the frozen...
-
667Lifestyle with Dog
7 Dog Gadgets To Make Your Life Easier
If you're looking for dog gadgets to make you and your furry friend's life...
-
641Skin & Coat
The 5 Best Dog Paw Balms For Your Furry Friend
To help keep your furry friend's paws in good shape and protected from a...
-
636FRONT PAGE
Family Is Heartbroken After They Found Out Their Missing Dog Got Hit By A Train And Buried In Shallow Grave
A family in Newtown, Sydney, Australia is left heartbroken after finding out their missing...
-
585About Breeds
Dogs With Dreadlocks: What Are Corded Dog Breeds?
Everywhere they go, dogs with dreadlocks always turn heads for their uniquely tangled appearance....